Last updated: December 6, 2025
If you’ve been battling nail fungus that keeps returning or refuses to budge, you may wonder whether the issue goes deeper than the nail. Many adults search for clear Signs of Internal Fungus only after weeks or months of frustration. This guide shows you how to recognize when stubborn nail fungus points to internal drivers—and what to do next.
For people who have tried creams, lacquers, or home remedies without lasting success, the possibility of an internal problem can feel alarming. You’re not alone. The good news is that identifying underlying contributors—like blood sugar issues, immune dysregulation, or circulation problems—often leads to more durable results and fewer recurrences.
In the following sections, you’ll learn how nail fungus starts, the red flags that suggest a systemic link, which medical conditions commonly overlap, how clinicians test for root causes, and practical steps to treat persistent nail infections from the inside out.
Key takeaways
- Stubborn or recurring nail fungus can signal internal contributors like blood sugar dysregulation, immune compromise, or poor circulation.
- Multiple nails on different limbs, systemic symptoms, or slow nail growth are key warning signs.
- Accurate diagnosis often requires lab tests, imaging for circulation, or metabolic screening.
- Addressing internal drivers plus surface care improves outcomes and reduces recurrences.
Keep reading to learn how to distinguish a surface-level infection from a deeper issue and how to build a plan that targets the true source of your nail problem for lasting relief.
Understanding Nail Fungus and Its Potential Internal Causes
Nail fungus (onychomycosis) begins when microorganisms—most often dermatophyte fungi, sometimes yeasts or molds—enter through microscopic cracks in the nail or surrounding skin. Warm, moist environments allow these organisms to thrive. At first, changes seem purely cosmetic. Over time, nails may thicken, crumble, or separate from the nail bed.
While external exposure is common, persistent infections can reflect internal factors that favor fungal growth or hinder defense. This is why different people exposed to the same locker room floor have different outcomes. When therapies fail repeatedly, it’s wise to consider an approach that goes beyond the surface and addresses the potential cause root, such as immunity or systemic drivers, rather than reusing creams that lack penetration.
What is nail fungus and how does it typically develop?
Nail fungus usually starts at the free edge or sides of the nail plate. Early signs include yellowing, white streaks, or subtle thickening. In a typical progression, the nail becomes more opaque, brittle, and distorted. The fungus can spread beneath the nail, making topical agents struggle to reach the live infection where it hides.
Think of the nail like a roof shingle. Once moisture and debris sneak under the shingle, surface sealants alone rarely restore integrity. Similarly, if the infection sits beneath the plate, superficial products can miss the target. That’s why some cases respond slowly or relapse after temporary improvement.
Common risk exposures include sweaty footwear, communal showers, nail salons with suboptimal sanitation, and minor trauma from tight shoes or running. Athletes, service industry workers, and people with long hours on their feet often notice initial changes after repeated friction. Addressing these mechanical and moisture factors early can help, but it may not be sufficient if internal contributors are present.
Where possible, getting a sample for microscopy or culture confirms the diagnosis. Not all discolored or thick nails are fungal. Psoriasis, eczema, trauma, or repeated manicures can mimic infection. Misdiagnosis leads to missed opportunities and delays in finding the true solution.
Can internal health conditions cause or worsen nail fungus?
Yes. Several internal conditions create a favorable environment for fungi to persist. Blood sugar dysregulation can feed fungi via excess glucose in tissues. Circulatory issues reduce nutrient and immune cell delivery to distal tissues like toes, slowing clearance. Autoimmune disease, immunosuppressive medications, and chronic stress can weaken defense and delay nail regrowth.
In clinical practice, we see patterns. People with prediabetes or diabetes experience more frequent and stubborn nail infections, often affecting multiple nails. Individuals on corticosteroids, chemotherapy, or biologics may find infections harder to eradicate. Thyroid disorders and nutritional deficiencies can alter nail growth, making nails slower to replace damaged tissue.
“When a nail infection resists reasonable topical care, look upstream. Glucose control, vascular health, and immune function commonly determine whether the fungus is a guest or a permanent resident.”
– Board-certified dermatologist
Importantly, internal contributors do not mean the infection came from “inside” first. Most start externally, but systemic factors decide severity and persistence. This distinction guides treatment: surface measures plus tailored internal correction yield better long-term outcomes than either approach alone.
Finally, yeast overgrowth in the body is often discussed online. While systemic candidiasis is uncommon outside specific immunocompromised contexts, localized yeast issues (e.g., in skin folds) can coexist with nail fungus. Thorough assessment distinguishes true systemic disease from local fungal colonization with internal risk amplifiers.
How do external vs. internal factors differ in nail infections?
External factors are about exposure and environment: wet socks, occlusive shoes, nail-salon trauma, or minor cuts. Internal factors are about your body’s ability to restrain fungal growth: blood sugar control, circulation, immunity, and nutrient status. These forces interact. High exposure can overwhelm even healthy nails; internal vulnerabilities magnify small exposures into chronic problems.
It’s also valuable to distinguish nail fungus vs yeast infection. Dermatophytes often cause classic nail thickening and yellow-brown discoloration, while yeast (Candida) may be more common in fingernails, especially with frequent wet work or chronic paronychia. Treatments overlap but can differ in drug selection and preventive steps.
| Factor | External Drivers | Internal Drivers | Practical Implication |
|---|---|---|---|
| Moisture/Heat | Sweaty socks, wet work, gym floors | Excessive perspiration from endocrine issues | Drying routines and breathable footwear matter |
| Trauma | Tight shoes, repetitive running impact | Slow nail growth under endocrine/nutrient issues | Reduce friction; support nail turnover |
| Immunity | — | Chronic stress, medications, illness | Screen risk; adjust treatments accordingly |
| Circulation | Cold, constrictive footwear | PAD, Raynaud’s, diabetes | Warmth, activity, vascular assessment |
| Organism Type | Dermatophyte exposure | Yeast overgrowth in wet environments | Lab confirmation guides targeted therapy |
Understanding which side of the equation dominates helps you prioritize. If your feet are perpetually damp, moisture control rises to the top. If nails grow very slowly and multiple infections recur, internal contributors deserve focused attention. Your plan can and should be personalized—most success comes from layering both.
Over time, addressing only one side can lead to cycles of improvement and relapse. Pairing adequate penetration at the nail with internal support increases the odds of durable clearance and reduces frustration.
Consider a simple, numeric benchmark: toenails often grow 1–2 mm per month. If your infected edge hasn’t advanced in 3–4 months despite care, slow growth and suboptimal delivery of treatments to the nail bed may be issues. That’s a cue to widen the evaluation beyond creams.
Finally, note that the longer a nail remains infected, the more the nail bed can change shape, making future treatments less effective. Early, holistic action protects nail architecture and reduces the risk of chronic changes.
Key Signs Your Nail Fungus May Be Linked to Internal Health Issues

Before diving into details, it helps to see the big picture. If you recognize several of these signs at once, your infection may be sustained by an internal driver rather than just external exposure. This quick list can guide your next steps and your conversation with a clinician.
Use the following as a screening framework. You don’t need all seven to justify deeper evaluation—two or three, sustained over months, often suffice. Keep notes with dates and photos; your timeline will help your provider decide on testing or referrals.
- Recurrence after seemingly successful treatment, especially within 3–6 months.
- Multiple nails on different limbs involved at the same time.
- Very slow nail growth or nails that appear to “stall.”
- Coexisting athlete’s foot, jock itch, or chronic skin yeast issues.
- Systemic symptoms: fatigue, frequent infections, tingling/numbness in feet, or leg cramps.
- History of prediabetes/diabetes, thyroid issues, anemia, or poor circulation.
- Topical treatments fail repeatedly, suggesting limited penetration or resistance.
Not every sign points to a dangerous condition, but the pattern matters. The more items you check, the stronger the case for a dual strategy—surface and internal—plus testing to rule out contributing conditions.
Remember: early action offers the best chance for clear nails and less time lost to trial-and-error solutions that don’t address the underlying terrain supporting the fungus.
Persistent or recurring nail fungus despite topical treatments
When a nail improves on the surface yet relapses within months, ask why. Sometimes the issue is inadequate dosing or duration; nails grow slowly, and treatment must outlast the infected portion. But frequent recurrences suggest the environment under the nail remains permissive, or penetration is inadequate for where the fungus resides.
Real-world example: A patient applies a medicated lacquer for 6 months and sees partial clearing. Two months after stopping, discoloration reappears. That relapse, despite meticulous hygiene, hints at an internal factor—like borderline blood sugar—or at a subungual reservoir that topical molecules could not reach reliably.
Look for compounding clues: recurrent athlete’s foot, itchy rashes in skin folds, or toenail changes after each marathon. Each clue points to either reinoculation from nearby fungal colonies or internal drivers that lower your antifungal resilience. Expand the plan accordingly to prevent the pattern from repeating.
Multiple nails affected on different limbs simultaneously
When both feet or a hand and a foot are involved at the same time, especially across three or more nails, consider systemic contributors. This distribution suggests a common internal vulnerability rather than a single external source or localized trauma. It’s less likely a one-off injury and more likely a body-wide susceptibility.
Circulation plays a major role here. The nails farthest from the heart receive less blood flow and immune surveillance. If you also have cold toes, leg cramps while walking, or slow-healing cuts, it’s reasonable to screen for peripheral artery disease or diabetes-related microvascular changes.
In practice, this pattern often benefits from a combination: antifungal therapy with systemic reach, footwear and moisture control, and internal support such as glucose optimization or vascular-friendly habits. Tackling all three layers reduces reinfection and accelerates progress.
Presence of additional systemic symptoms alongside nail fungus
Pay attention to your whole-body signals. Fatigue, unintentional weight changes, increased thirst, tingling or numbness in the feet, frequent skin infections, or slow wound healing are systemic clues that may accompany stubborn nail fungus. These symptoms don’t prove a severe disease, but they warrant evaluation.
For example, a person with borderline A1C and frequent nighttime urination might also notice chronic athlete’s foot and recurring toenail issues. This triad increases suspicion of an internal glucose regulation problem. Similarly, frequent sinus infections or slow recovery from colds might reflect immune challenges that make clearing nail infections harder.
Track these symptoms over time. A two-week episode might be coincidence, but three months of patterns invites investigation. Bring your notes to your provider; specific timelines help target the right tests and reduce guesswork.
Medical Conditions Commonly Associated with Nail Fungus
Nail fungus clusters with several health conditions that interfere with immune function, circulation, or tissue integrity. Recognizing these connections doesn’t mean every thick nail signals a disease. It means that evaluating the context can lead to smarter, faster solutions.
Below, we examine diabetes, immune compromise, and poor circulation. You’ll learn how each condition affects nail biology, why it raises relapse risk, and what practical steps can mitigate that risk while improving overall well-being.
How does diabetes increase susceptibility to nail fungus?
Diabetes and prediabetes alter skin and nail environments through several mechanisms. Elevated glucose supports fungal growth, while microvascular changes reduce immune cell trafficking to distal tissues. Nerve changes can blunt the sensation of minor injuries, allowing unnoticed trauma that opens the door to infection.
Clinically, people with diabetes often present with multiple nails involved, coexisting athlete’s foot, and slower response to standard treatments. Nail growth may be delayed, and minor pressure points from shoes can trigger persistent skin breakdown—another infection source. This is why foot care is a mainstay of diabetes management.
Action steps include optimizing A1C, choosing moisture-wicking socks, rotating footwear, and checking feet daily. If fungal infection is confirmed, your clinician may prefer systemic therapy when appropriate, paired with topical support to reduce reinoculation. Regular podiatry visits help prevent complications.
Numbers matter. Even a modest A1C reduction can improve tissue quality and immune efficiency. Over 6–12 months, better glucose control often correlates with improved nail appearance and fewer fungal flares, especially when combined with evidence-based antifungal regimens.
Is compromised immunity a risk factor for persistent nail fungus?
Yes. Immunocompromise—whether from conditions like HIV, medications like corticosteroids or chemotherapy, or autoimmune diseases—can delay fungal clearance. The nail plate acts as a barrier that already slows drug penetration; when immune support is reduced, fungi gain a persistence advantage.
However, not all immune compromise is obvious. Chronic stress, poor sleep, low vitamin D, or micronutrient deficiencies can subtly shift immune balance. People in high-pressure jobs who sleep five hours per night often report recurring skin and nail issues that improve with lifestyle changes and targeted supplementation guided by labs.
Partnering with your care team is essential. If you take immunosuppressants, your prescriber can advise on safe antifungal options and timing relative to other treatments. Non-drug strategies—like moisture control, footwear hygiene, and nail debridement—become even more important to reduce microbial load.
Remember, the goal is not just killing fungus; it’s restoring a nail environment where fungus cannot easily return. That requires aligning external measures with your unique immune context.
Over time, consistent small steps—better sleep, stress reduction, nutrient optimization—stack up. They won’t replace antifungals when needed, but they raise your antifungal “ceiling,” improving the odds that treatments succeed.
Can poor circulation be an underlying cause for nail infections?
Reduced blood flow to the feet limits delivery of immune cells and medications. In peripheral artery disease (PAD) or diabetes-related vascular changes, nails may grow slowly and become more vulnerable to infection. Cold toes, leg cramps with walking, and slow wound healing are common clues.
Practical measures include daily walking (as tolerated), calf raises, leg elevation after long sitting, avoiding tight socks, and keeping feet warm without trapping moisture. Clinicians may order an ankle–brachial index (ABI) test to screen for PAD or refer to a vascular specialist if symptoms warrant.
In people with vascular issues, professional nail debridement to reduce thickness helps topical agents reach the source. Treatment durations may be longer, and systemic options considered, depending on overall health and medication interactions. Preventing trauma from ill-fitting shoes becomes a priority to avoid secondary bacterial infections.
Think of circulation as the delivery truck for your antifungals and immune helpers. If the truck gets stuck in traffic, the package arrives late or not at all. Improving traffic flow makes every other part of the plan work better.
Diagnosing the Root Cause: When to Suspect an Internal Problem
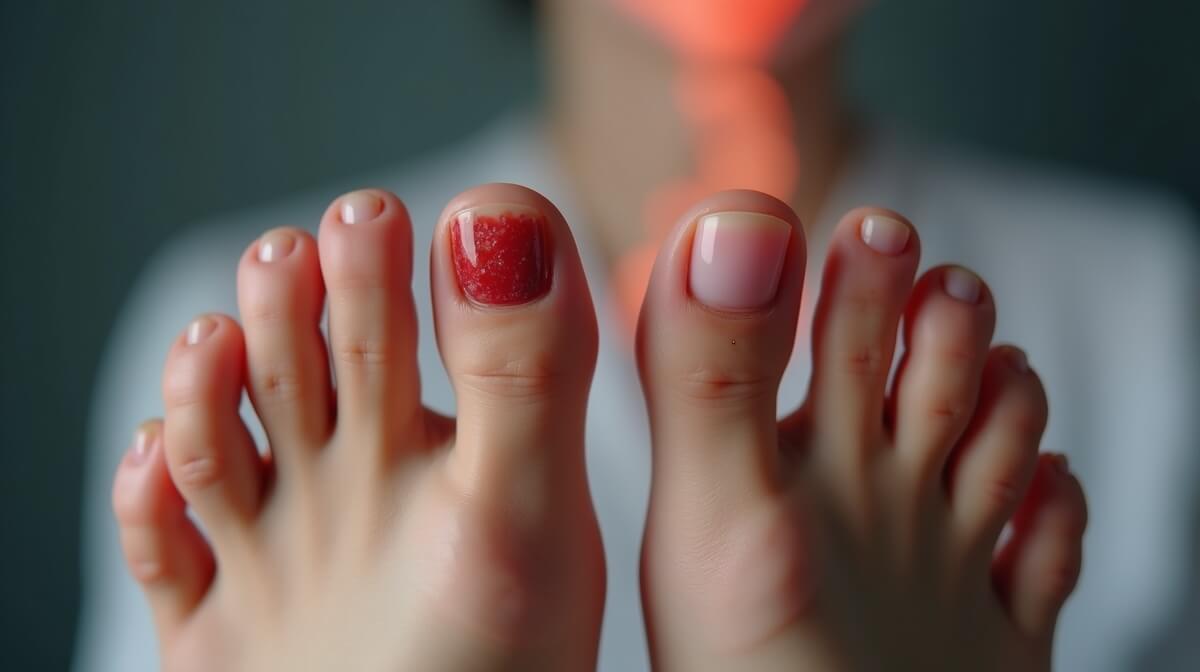
Good diagnosis prevents wasted time and money. If your nail has resisted thoughtful care, it’s reasonable to differentiate a surface-dominant problem from one with internal drivers. Below are the tests and clinical steps commonly used to do that safely and efficiently.
Importantly, testing is not about “proving” you did something wrong. It’s about identifying the variables that keep the fungus comfortable. Remove those variables, and treatments become more effective.
What tests help determine internal vs. external causes of nail fungus?
Start with confirming the organism. Your provider may obtain a nail clipping or scraping for microscopy (KOH prep), PAS stain, culture, or PCR. These tests clarify whether you’re dealing with dermatophytes, non-dermatophyte molds, or yeast—each may guide medication choices and expectations.
Next, screen for internal contributors guided by your history. Common labs include fasting glucose, A1C, lipid panel, thyroid function, iron studies, B12, vitamin D, and sometimes inflammatory markers. For circulation, an ABI test helps detect PAD; if neuropathy symptoms are present, your clinician may assess for peripheral neuropathy.
Imaging is rarely needed for straightforward nail fungus but may be considered if there’s concern for bone involvement in severe cases or if recurrent infections suggest structural abnormalities. Dermatology or podiatry referrals are useful when the diagnosis is uncertain or when nails are highly thickened and require debridement.
Interpreting these results in context ensures you’re not over- or undertreating. For example, a normal A1C with a low ferritin could shift focus to iron and nail growth support rather than glucose control. The goal is a targeted, not generic, plan.
When should you consult a doctor for persistent nail problems?
Seek medical advice if any of the following apply for 8–12 weeks: no improvement despite consistent topical therapy, spreading to multiple nails, significant pain, or nail lifting with debris underneath. Also consult promptly if you have diabetes, symptoms of poor circulation, or immune compromise of any kind.
Other red flags include new dark streaks under the nail, rapid nail destruction, or bleeding with minimal trauma. These are not typical of routine fungal disease and require professional evaluation to exclude other diagnoses, including melanoma in rare cases.
If cost is a concern, start with your primary care clinician, who can confirm the diagnosis and order initial labs. Telehealth options may be available for follow-up. Podiatrists and dermatologists provide specialized care for complex or recalcitrant cases and can perform in-office debridement to speed topical entry.
Documenting your treatment history—names of products, how often you applied them, and for how long—helps your provider avoid repeating ineffective strategies and accelerates progress to the next best step.
How to communicate symptoms and concerns to a healthcare provider
Arrive with a brief timeline that includes when you first noticed changes, treatments tried, and any triggers (e.g., marathon training, new job requiring safety boots). Note any systemic symptoms, like fatigue or increased thirst, and your family history of diabetes or thyroid disease.
Bring clear photos taken in consistent lighting every four weeks. Visual documentation helps differentiate true worsening from normal nail shedding. Mention workplace exposures, gym habits, and salon practices. These details often inform prevention, even if internal factors are present.
Ask direct questions: “Is my infection mainly external or are internal factors likely?” “Which tests would clarify that?” “How will we measure progress?” Clear questions signal that you’re invested in outcomes and open the door to collaborative planning.
Finally, discuss your priorities—cosmetic improvement for a wedding in six months, pain relief to resume running, or minimizing drug interactions. Aligning the plan with your goals improves adherence and satisfaction.
Addressing Nail Fungus by Targeting Internal Issues
Effective treatment usually involves two lanes moving in parallel: local control at the nail and systemic support to change the conditions that allow fungi to persist. When both lanes move together, results accelerate and recurrences drop.
Below, we outline lifestyle measures, medical therapies, and relapse prevention tailored for people with underlying contributors. Your clinician can help you adapt these steps to your health status and preferences.
Which lifestyle changes can support healthy nails from the inside out?
Start with moisture and friction control. Rotate two or three pairs of shoes to let each dry fully, use moisture-wicking socks, and change them after workouts. After showering, dry between toes with a clean towel or cool hairdryer setting. These simple steps reduce the fungal “fuel” source—warmth and dampness.
Address nutrition that supports nail growth and immune function. Aim for steady blood sugar with balanced meals (protein, fiber, healthy fats). Ensure adequate iron, zinc, biotin, and vitamin D through diet or clinician-guided supplementation. If you have GI symptoms, discuss evaluation for absorption issues that could affect nutrient status.
Daily movement improves circulation to the extremities. Even 10-minute walks after meals help glucose control and blood flow. Foot-specific exercises—like toe curls and calf raises—help too. Prioritize 7–9 hours of sleep to support immune balance, and set consistent wake times to stabilize circadian rhythm.
- Rotate footwear; disinfect insoles; sun-dry shoes when possible.
- Wash and dry feet nightly; apply an antifungal powder to shoes.
- Trim nails straight across; avoid cutting corners too deeply.
- Add two post-meal walks; elevate legs after long sitting.
- Schedule lights-out 30–60 minutes earlier to improve sleep quality.
Consider a realistic time horizon. Toenails can take 9–18 months for complete replacement; fingernails 4–6 months. Set milestones every 8–12 weeks rather than daily checks. Measure progress by new clear growth at the cuticle advancing outward, not by instant color change at the tip.
Finally, coordinate with your clinician if you’re on medications that interact with antifungals. A shared plan on timing, doses, and monitoring reduces risks and increases confidence in your strategy.
Medical treatments for nail fungus with suspected internal origins
When internal contributors are suspected, medical therapy often includes systemic antifungals (when safe), supported by local measures. Oral agents can reach the nail bed through the bloodstream, improving penetration for subungual infections. Your clinician will weigh benefits against potential liver or drug interaction risks.
Topical options—medicated lacquers or solutions—still play a role, especially after mechanical debridement by a professional. Debridement thins thick nails, allowing better topical reach. In some cases, pulse dosing strategies or combination regimens may be used to balance efficacy and safety.
Adjunctive approaches may include managing athlete’s foot aggressively to prevent reinfection, treating household contacts with symptoms, and disinfecting nail tools at home. Some people explore diet changes, probiotics, or essential oils; if you’re considering alternatives, see our review of a deep-acting solution that discusses penetration challenges and the importance of targeting the suspected internal “root cause” rather than masking surface discoloration alone.
Criteria for escalation include severe thickening that impairs walking, pain, or infections resistant to reasonable topical trials. Your provider may recommend a course of systemic therapy with lab monitoring or, in rare scenarios, consider partial nail procedures for recalcitrant segments.
Set clear checkpoints. For example, expect to see a 1–2 mm band of clear growth from the cuticle by 8–12 weeks. If not, reassess for adherence, reinoculation sources, or unaddressed internal factors like glucose control or circulation.
“Success improves when we match the treatment to the biology—debride thick nails, strengthen circulation, optimize glucose, and use antifungals long enough to outgrow the infected plate.”
– Podiatry specialist
Remember that medication choice can differ by organism. Dermatophytes often respond to specific systemic agents, while Candida species may require alternatives. Confirming the organism prevents trial-and-error and avoids unnecessary exposure to drugs that won’t help your specific case.
Communication is key. Share any side effects early, and keep a simple log of doses and applications. Adjustments in real time often rescue a plan before momentum is lost.
How to prevent recurrences in people with underlying health conditions
Preventing relapse is a marathon, not a sprint. Once you’ve gained clear new growth, taper your regimen thoughtfully rather than stopping abruptly. Many clinicians advise continued topical maintenance 2–3 times weekly for several months to protect the new plate during regrowth.
Footwear hygiene remains a cornerstone. Use antifungal shoe sprays or UV sanitizers; replace old, worn shoes that retain moisture. Launder socks hot and dry thoroughly. Keep separate clippers for infected nails and disinfect metal tools after each use with 70% isopropyl alcohol for at least one minute.
If you have diabetes or prediabetes, schedule routine foot checks and maintain A1C goals. For circulation concerns, keep walking and avoid tobacco exposure. For immune challenges, anchor sleep and stress practices to support your body’s defensive baseline.
Finally, build a quarterly review habit: take photos, note any color shift, thickening, or debris. Catching early changes allows quick interventions—often a short topical “booster”—instead of a full relapse.
Risks of Ignoring Internal Causes of Nail Fungus
Leaving internal contributors unaddressed can trap you in an expensive loop of temporary improvement and relapse. It also increases the risk of complications beyond the nail. Understanding these risks helps you decide when it’s time to widen the scope of care.
Fortunately, most complications are preventable with timely evaluation and consistent habits. Early recognition paired with targeted therapy protects nail structure and supports overall health.
What complications can arise from untreated internal problems?
Thickened nails can deform the nail bed, making future treatments less effective and causing discomfort in shoes. Recurrent fungal reservoirs in shoes or skin can seed new infections repeatedly. In people with diabetes or vascular disease, breaks in skin integrity raise the risk of bacterial infections like cellulitis.
Chronic pain or embarrassment can limit physical activity and social participation, which indirectly worsens circulation and metabolic health. That reduction in movement can loop back into poorer nail growth and higher infection risk—a vicious cycle that begins with a “cosmetic” problem.
There’s also the cost burden: repeated purchases of topicals that never fully reach the target, lost work time for appointments, and the mental load of ongoing frustration. A root-cause approach may look more involved, but it often saves time and money over the long arc of recovery.
Lastly, rare but serious conditions can masquerade as simple nail fungus. Prompt evaluation of atypical features prevents dangerous delays. When in doubt, get a culture or biopsy—certainty is your ally.
How delayed diagnosis impacts nail health and overall well-being?
The longer a nail remains infected, the more the nail architecture can change. Curvature increases, debris accumulates, and the nail may lift. This complicates shoe fit and daily comfort. Delays also allow fungal reservoirs to expand in footwear and nearby skin, turning a single-nail issue into a multi-nail challenge.
On the systemic side, delays can postpone the discovery of contributors like dysglycemia or vascular insufficiency. Early management of these conditions improves not only nail outcomes but also cardiovascular and metabolic health—benefits far beyond appearance.
In short, timely diagnosis narrows the gap between effort and results. Instead of chasing symptoms, you’ll be working a plan that makes each therapy more effective, compounding your gains month by month.
Consider setting a personal deadline—if there’s no meaningful progress in three months, escalate evaluation. That simple rule of thumb keeps momentum on your side.
Frequently Asked Questions About 7 Signs Your Nail Fungus is an Internal Problem
What are the main signs that nail fungus is due to an internal problem?
Look for patterns rather than a single symptom. Key signs include recurrence after topical success, multiple nails on different limbs, very slow nail growth, coexisting athlete’s foot or skin yeast, systemic symptoms (fatigue, tingling), a history of blood sugar or circulation issues, and repeated failures of topical therapy. When two or more persist over months, evaluate internal contributors and pair local care with systemic support.
How do I know if my nail fungus is related to diabetes or another health condition?
Consider your personal and family history, plus symptoms like frequent urination, increased thirst, slow-healing cuts, leg cramps, or numbness. Multiple nail involvement or repeated relapses raise suspicion. Your clinician can order A1C, fasting glucose, lipid panel, and an ankle–brachial index if circulation is a concern. Combining lab results with your nail history clarifies whether internal conditions contribute.
Can immune system disorders cause recurring nail fungus?
Yes. Autoimmune conditions and immunosuppressive therapies can lower antifungal defenses and slow nail regrowth. Even subtler factors—poor sleep, chronic stress, low vitamin D—can tip the balance. If you have immune-related issues, work with your care team on an integrated plan: tailored antifungals, moisture control, debridement, and sleep/stress/nutrition strategies to raise your antifungal resilience and reduce relapses.
Why doesn’t my nail fungus go away with OTC creams or topical treatments?
Topicals may struggle to penetrate thick, subungual infections, and treatment often stops too soon for slow-growing nails. Recurrence within months suggests a persistent reservoir or internal contributors like blood sugar or circulation challenges. Debridement improves penetration, and addressing internal factors improves durability. Confirming the organism type also matters because yeasts and molds may respond differently than dermatophytes.
Are there systemic symptoms to watch for with nail fungus?
Yes. Fatigue, frequent infections, increased thirst, night urination, leg cramps with walking, tingling or numbness in the feet, and slow wound healing can accompany persistent nail fungus. These don’t prove a serious illness but signal the need to evaluate for diabetes, thyroid issues, anemia, vitamin deficiencies, or circulation problems that may sustain the fungal environment.
How can medical tests differentiate between internal and external nail infection causes?
Lab confirmation (KOH, PAS, culture, PCR) identifies the organism and rules out look-alikes. Metabolic panels (A1C, fasting glucose, thyroid function, iron studies, vitamin D) reveal internal contributors. An ankle–brachial index screens circulation. When external factors dominate, tests are often normal. When internal drivers exist, targeted abnormalities guide treatment priorities and improve outcomes.
Should I see a podiatrist or a general physician for chronic nail fungus?
Start with your primary care clinician for diagnosis and initial labs to screen internal contributors. A podiatrist is ideal for nail debridement, footwear guidance, and advanced local care. Dermatologists help with complex or unclear cases. Many patients benefit from a team approach: primary care for systemic assessment and podiatry or dermatology for nail-focused procedures and therapies.
Do underlying health issues make nail fungus harder to treat?
Often, yes. Blood sugar dysregulation, immune compromise, and poor circulation lower your antifungal “ceiling,” making standard therapies less effective and relapse more likely. Recognizing and treating these contributors—while maintaining local measures—raises that ceiling. The result is better response, shorter total treatment time, and fewer recurrences over the long term.
Can poor circulation contribute to stubborn nail fungus?
Yes. Limited blood flow reduces delivery of immune cells and medications, slowing recovery and encouraging relapse. Clues include cold toes, calf pain with walking, and slow-healing cuts. Screening with an ankle–brachial index and adopting circulation-friendly habits—regular walking, leg elevation, warm (not sweaty) feet—help treatments work better and reduce persistence.
What lifestyle changes help prevent nail fungus if I have chronic health conditions?
Combine moisture control (sock changes, shoe rotation), foot hygiene, and nail trimming with systemic support: balanced meals for glucose stability, nutrient optimization (iron, zinc, vitamin D), consistent sleep, and daily movement to improve circulation. Maintain topical maintenance for several months after clearing. These habits create an environment less hospitable to fungi and protect your progress.
What complications can occur if an internal cause of nail fungus is ignored?
Untreated contributors increase relapse risk, nail thickening, deformity, pain, and footwear problems. In diabetes or vascular disease, skin breaks can invite bacterial infections. Delays can also postpone diagnosis of metabolic or circulatory conditions affecting overall health. Addressing root causes early reduces these risks and typically shortens total treatment duration.
Is nail fungus ever a sign of a more serious or undiagnosed internal disease?
Usually, nail fungus is a localized infection. However, persistent, multi-nail disease—especially with systemic symptoms—can be the first visible clue of issues like prediabetes, diabetes, thyroid disease, anemia, or circulation problems. While serious systemic fungal disease is rare outside specific contexts, it’s prudent to screen when patterns suggest internal involvement.
Conclusion
Stubborn nail fungus is more than a cosmetic annoyance. When it returns after treatment, involves multiple nails, or coexists with systemic symptoms, it may be pointing to internal contributors—blood sugar balance, circulation, or immune tone—that keep the infection comfortable. Addressing both the nail and the whole-body context gives you the best chance at clear, resilient nails.
Use the seven signs as your roadmap, confirm the organism, and ask for targeted labs when patterns persist. Pair professional debridement and evidence-based antifungals with moisture control, shoe hygiene, and metabolic support. With a realistic timeline and a plan that tackles the root cause, progress becomes visible and sustainable. → Click here to read our analysis of a solution that focuses on the “root cause.”
In summary
- Look for recurrence, multi-nail spread, slow growth, and systemic clues to flag internal drivers.
- Confirm the organism and screen for glucose, circulation, thyroid, iron/B12, and vitamin D.
- Combine debridement, antifungals, and lifestyle to prevent reinfection and support nail regrowth.
- Set 8–12 week checkpoints and a 3-month escalation rule if progress stalls.
Did this help? Share your experience, drop your questions, and pass this guide to someone frustrated with recurring nail fungus—small insights can lead to lasting results.
Important Health Notice and Disclaimer: This guide is educational and not a substitute for personalized medical advice, diagnosis, or treatment. Always seek the guidance of your physician, dermatologist, or podiatrist with any questions regarding a medical condition or therapy. If you have diabetes, circulatory problems, immunosuppression, severe pain, spreading infection, or dark streaks under the nail, seek prompt in-person evaluation. Medication decisions—including antifungals—must consider your health history, labs, and potential drug interactions.













Add comment